Kaitlin Sullivan –
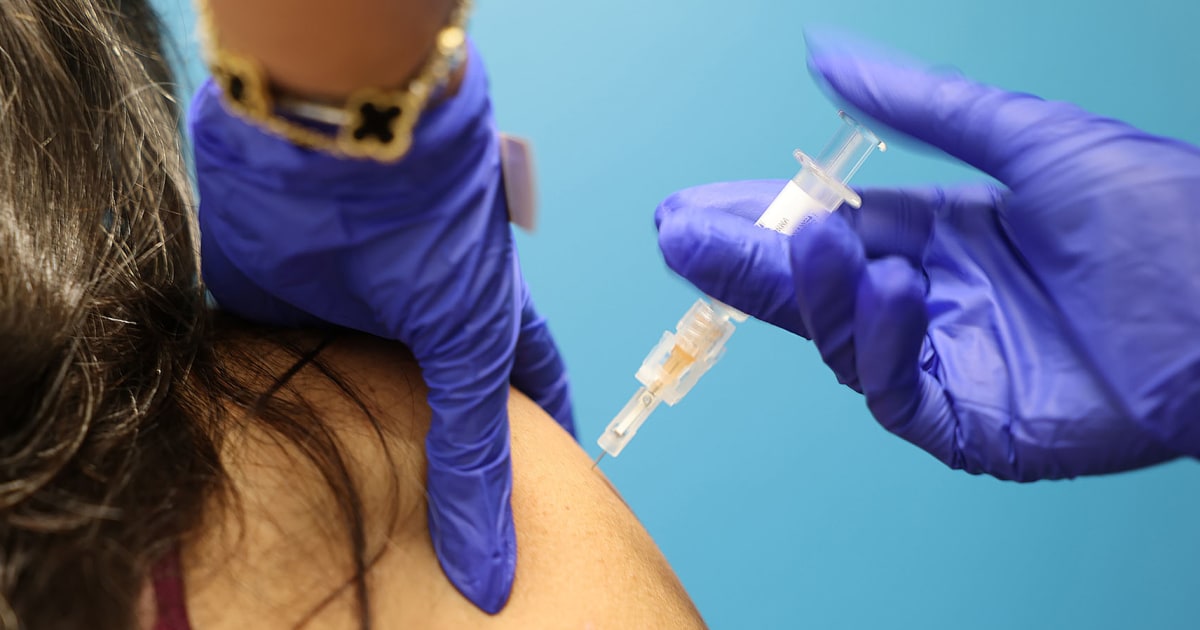
COVID-19 vaccines could have an unusual benefit that has nothing to do with the virus they are designed to combat: stimulating the immune system to better attack tumors during cancer treatments.
This is indicated by new research results presented Sunday in Berlin, Germany, at the European Society of Medical Oncology conference. The study is still in its early stages, as it has not yet been tested in a phase three clinical trial, but experts say it shows promise.
“I’m cautiously optimistic,” said Stephanie Dougan, an associate professor of cancer immunology and virology at Dana-Farber Cancer Institute, who was not involved in the research. “There is a scientific logic to why this might work.”
Researchers found that among cancer patients treated with immunotherapy, those who received an mRNA COVID-19 vaccine within 100 days before starting treatment lived longer.
Only about 20% of patients on immunotherapy, which harnesses the immune system to fight cancer cells, respond to treatment. Finding a way to increase the effectiveness of medications has been a feat that researchers have been exploring for years without success.
In general, the immune stimulation tactics used until now have been excessive or insufficient to activate the immune system, causing an exaggerated response that can harm the body. There is a chance that COVID-19 mRNA vaccines could fall somewhere in between.
“Maybe we just needed something that was medium intensity, and this could be it,” said Dougan, who stressed the need for further research.
(The CDC endorses COVID-19 vaccines but now recommends checking with doctors first.)
That research will get underway soon: Dr. Adamres Grippin, a senior resident in radiation oncology at the University of Texas MD Anderson Cancer Center, who co-led the study, said his team will begin a phase three clinical trial to confirm the initial results.
In the research presented Sunday, Grippin and his co-authors analyzed the survival rates of more than 1,000 people with advanced non-small cell lung cancer who were treated with immunotherapy between 2019 and 2023. Of them, 180 received an mRNA vaccine against COVID-19 within 100 days of starting treatment.
The group’s average survival time — when half of those who underwent treatment are still alive — was almost twice as long for those who got vaccinated compared to those who didn’t: about three years versus just over a year and a half.
The researchers also compared survival rates in a smaller group receiving immunotherapy for metastatic melanoma: 43 received a COVID-19 mRNA vaccine; 167 no. For those who were not vaccinated, average survival rates were just over two years. Those vaccinated before treatment had not yet reached their median survival point after more than three years of follow-up.
In other experiments with mice, the researchers obtained a response that they believe matches the effect of vaccines in humans.
“It greatly stimulates the immune system against tumors,” Grippin said.
a hope
Vaccines using mRNA are already a promising area of cancer research. Scientists have developed personalized mRNA-based disease vaccines that are tailored to target each person’s specific tumor, as well as others that target genes commonly found in certain types of cancer, such as pancreatic cancer.
These advances occur as the Donald Trump Administration has canceled $500 million in funding for research into mRNA vaccines against infectious diseases.

If Grippin’s next trial confirms the results of early research, it could represent the next frontier for research into mRNA vaccines and cancer.
Immunotherapy drugs work by boosting the immune system’s ability to fight cancer, often by increasing the power of immune cells called T cells that attack invaders, or making it easier for them to find tumors.
The mouse part of the new research found that the COVID-19 mRNA vaccine appeared to help the immune system be better prepared to recognize tumors as a threat by stimulating dendritic cells, a type of white blood cell. When they detect a threat, they activate a kind of beacon that guides T cells toward the perceived invader so they can attack it.
(The CDC endorses COVID-19 vaccines but now recommends checking with doctors first.)
However, not all people have T cells capable of fighting tumors naturally, so scientists believe that immunotherapies only work in some cancer patients who receive them. In these, the immune system recognizes cancer cells as a threat, but its specific T cells are unable to stop the growth of tumors.
“It’s just a matter of chance whether you have those cells or not,” explained Jeff Coller, a professor of RNA biology and therapeutics at Johns Hopkins Medicine, who was not involved in the research.
Getting a COVID-19 mRNA vaccine doesn’t change whether a person has the specific T cells needed to fight their tumors, but it does appear to increase the likelihood that dendritic cells will detect a tumor as a problem and direct T cells toward the tumor.

If those cells are programmed to kill tumor cells, an mRNA vaccine that activates the target before the person begins immunotherapy can boost their immune system and help make treatment more effective.
Coller said one of the reasons mRNA technology may be the best tool to elicit this response is because all cells already contain mRNA.
“We are taking advantage of that natural process that your body already knows how to respond to,” he said. “You are using your body’s natural system to fight tumors.”
(The pandemic aged our brains, whether we had COVID or not, study finds)
Dougan said it’s possible that other factors influenced the longer survival of vaccinated people before immunotherapy treatment. For example, a COVID-19 infection could have weakened an unvaccinated person’s body and impaired its ability to fight cancer cells. Preliminary studies like this have already shown promising results that have not been confirmed in subsequent trials.
“Retrospective studies have fooled us before,” he said. Grippin agreed that the findings deserve further analysis.
“These data are exciting, but all of these findings must be validated in phase three clinical trials to determine if these vaccines should be used in our patients,” he insisted.