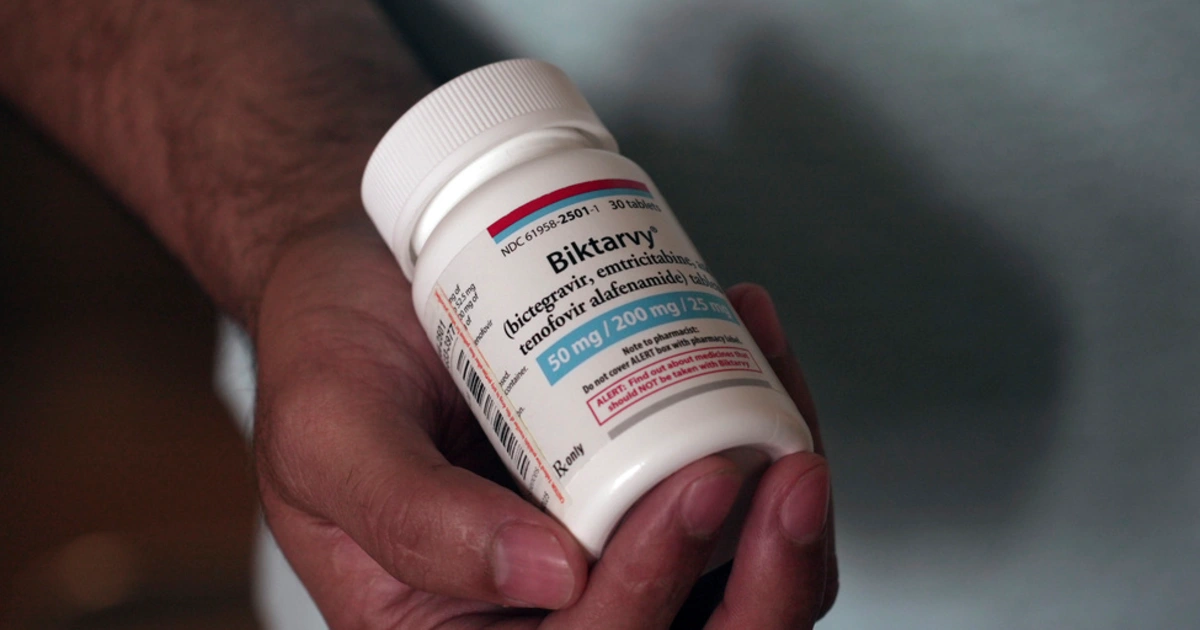
March came with anguish for Agustín: starting this month he will no longer receive the free medication that has allowed him to reduce his viral load to undetectable levels and without which his life and health are at risk.
He, a 34-year-old man living with HIV who asked not to reveal his last name due to the stigma associated with the virus, is one of the more than 12,000 people who had access to free treatment and assistance paying insurance premiums in Florida through the AIDS Drug Assistance Program (ADAP) and that as of March 1 they no longer qualify for these benefits after the state Department of Health adjusted the requirements.
Among the changes are a new maximum income limit (from about $63,000 to just over $20,000), a reduction in assistance to cover health insurance costs and the removal of Biktarvy, the most prescribed antiretroviral nationally, from its approved list of prescription drugs.
(Republicans seek deep cuts in funding for HIV prevention and treatment)
But Florida is not the only one: almost twenty states have implemented smaller-scale adjustments to their ADAP, according to data from the nonprofit organization NASTAD, which attributes this to an increase in the costs of care and more people needing it, while federal funds have remained almost unchanged over the last decade.
At least 18 states already have measures in place ranging from reduced funding for basic medical services, spending limits, or restrictions on help paying insurance premiums. Others are considering establishing waiting lists, something that, according to a Kaiser Family Foundation analysis, had not been considered in recent years.
“We are talking about something that has a direct impact on my health,” Agustín told Noticias Telemundo. “Thanks to having that treatment, thanks to having that follow-up by a doctor, I have remained undetectable for all this time,” he said.
That has allowed him to work and make future plans such as studying, he said. Now he will have to pay almost $300 a month — 10% of the annual income for him, who earns about $15,000 more than the new limit — for health insurance that he still doesn’t know for sure what it will cover.
“It’s not that they made things a little more flexible,” he said, “but that they were radical to leave out the majority of HIV-positive patients and save them that money, I guess.”
(The FDA approves a vaccine for HIV prevention that demonstrated great effectiveness in clinical trials)
The Florida Department of Health announced the changes in January, saying they will “avoid a deficit of more than $120 million” for the state and that it “remains committed to providing services through this vital program.” The department did not immediately respond to a request for comment.
Patients, congressmen and non-profit organizations such as the AIDS Healthcare Foundation (AHF) have criticized the measure, claiming that it will cause a “public health crisis,” since reducing the virus to undetectable levels in a person also prevents them from sexually transmitting it to others.
Impact on health
“Eventually the virus will begin to reproduce again,” Dr. Jon Appelbaum, a specialist in internal medicine and HIV treatment, explained to Noticias Telemundo.
Although getting it to undetectable levels takes time, “for most people, in a matter of a week or more, we will be able to detect the virus in the bloodstream again” when they stop treatment, he said.
“And you run the risk of developing what we call opportunistic infections that can put you in the hospital and you can even die from these infections,” he warned.
His immune system “is being devastated.”
In the end, “the overall effect will be that this will increase health care costs,” he explained. They can also sexually transmit the virus to someone else.
“The clinical medical consequences of not taking your medications are enormous,” stressed Esteban Wood, political and advocacy director of AHF, an organization that sued the Department of Health in Florida to try to stop adjustments to the program.
According to Wood, it is possible that some people continue the medications intermittently which can lead to “experiencing resistance.”
He estimates that without health insurance, treatment can cost more than $4,000 a month. This is without counting the laboratory tests or control appointments that patients like Agustín received for free.
“If I make $25,000 a year, now I have to make an impossible decision to pay my rent, pay for my housing, or pay for life-sustaining medications?” Wood said.
Other states prepare for changes
Although Florida is the state with the most radical changes, Pennsylvania, Kansas, Delaware and Rhode Island also adjusted the income level for beneficiaries, affecting another 2,000 people.
That’s not counting the states that are considering implementing new measures such as waiting lists and eligibility requirements.
Federal funding for assistance programs, which are part of the Ryan White Care Act, “has remained virtually unchanged over the past decade,” NASTAD mentioned among the reasons cited by states for the changes.
This while “customer enrollment and healthcare costs, including prescription drug expenditures, insurance premiums and cost sharing, have continued to increase,” he said.
Dr. Appelbaum said these are “life-saving” programs aimed at people who have no other way to pay for their treatment.
State legislators in Florida are working on a bipartite solution, Democratic Senator Carlos Guillermo Smith confirmed to Noticias Telemundo, who said they are looking for financing alternatives… but that could take a while.
“Cutting the ADAP is not only cruel, but short-sighted,” the state legislator said in a statement in which he indicated that the human cost “is enormous and the financial cost to our health system will only increase.”
For Agustín it is about his life.
“In the end we are talking about a disease that although you can live with it for a lifetime, you need treatment and follow-up to be able to continue living.”